Attention is being paid nationwide to the potential of data interoperability to support better health care, yet HCOs can still maximize their data without waiting on their EHR system to overcome its challenges.
Integrating data from a wide range of sources can improve both patient care and the bottom line.
What is data interoperability? According to the nonprofit Data Interoperability Standards Consortium:
Data interoperability addresses the ability of systems and services that create, exchange and consume data to have clear, shared expectations for the contents, context and meaning of that data.
What role does it play in health care? As health care organizations (HCOs) rely more and more on electronic health records (EHRs), it’s clear that there’s an advantage to having access to details about a patient’s health history from a wide range of sources.
For instance, a recent survey explored the relationship between the interoperability of data within health care systems and the quality of patient care. The survey was conducted by the Healthcare Financial Management Association and sponsored by Humana, a leading domestic health insurance provider.
Of the HCO financial leaders surveyed, 74 percent expressed their belief in the importance of integrated data for quality patient care. They are recognizing that constant and accurate exchange, transmission, and communication of data across systems is fundamental to their operations.
The quality integration of health data systems is essential for patients with chronic conditions. Patients with more serious illnesses often require engagement with several specialists, which means it’s particularly important for the findings and data from each specialist be succinctly and properly communicated to fellow doctors and care providers within and outside of the HCO.
Why Interoperability Matters With Health Care Data
- It can improve patient safety and quality because it allows providers to spend more time on patient care rather than chasing down information among disparate systems.
- It should reduce medical errors.
- It enhances operational efficiencies by providing clinicians all the patient information they need to quickly define treatment.
- It contributes to better continuity of care since the patient’s information is available to clinicians throughout episodic and longitudinal care journeys.
- It can reduce cost by reducing the time and effort required to acquire and share patient data.
The Challenges of Interoperability
HCO’s interoperability initiatives are being impeded by their EHR systems. Their data challenges have only been worsening with the explosive growth of health information, and the speed at which it is created.
EHR vendors have been committing to and demonstrating open and interoperable initiatives, but despite that, the simple fact that interoperability still doesn’t really exist raises the question: Why has their pace and progress on solving interoperability been stagnant?
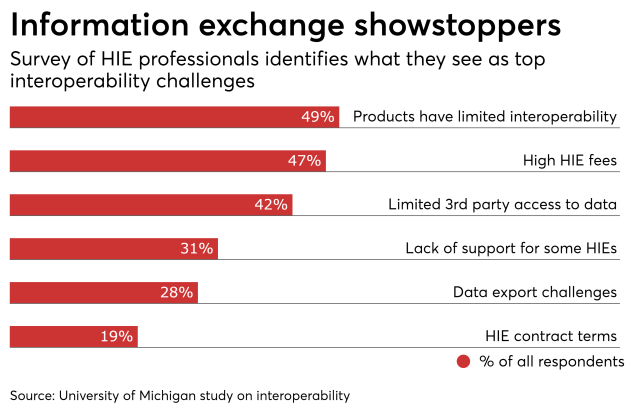
Health Information Exchange (HIE) professionals identify information blocking by their vendors as a primary challenge to interoperability.
The impact of their performance is easy to see. Even the most sophisticated HCOs struggle to overcome interoperability barriers. The time and investment it takes to accomplish this aren’t possible or sustainable for many organizations. For them, interoperability is more often a goal rather than a reality.
So, with all the federal attention and all the groups focused on interoperability, and all the time invested in developing health IT standards, why haven’t EHR vendors invested interoperability with the same strategic importance they’ve given other differentiating enhancements they’ve brought to market in recent years?
It Doesn’t Take Interoperability to Maximize Your Data
d2i specializes in the acquisition and integration of data from multiple source systems for operational efficiency and quality of care. We take all of your data — not just your EHRs — cleaning and normalizing it for easy analysis. d2i’s cloud-based performance analytics solutions give your clinical department stakeholders the information they need to make the best decisions for patients and to improve their performance.
To learn more about how we can help put your data to work, schedule a 30-minute demo with one of our business intelligence experts.
